WVU Medicine Children’s first in the state to offer new neonatal cardiac intervention
MORGANTOWN, W.Va. – Shani Berry of Fayette County was admitted to the hospital the Saturday before her water broke unexpectedly on May 17. She was only 26 weeks along in her pregnancy.
“I was so nervous,” she said. “We had been trying for a long time to grow our family.”
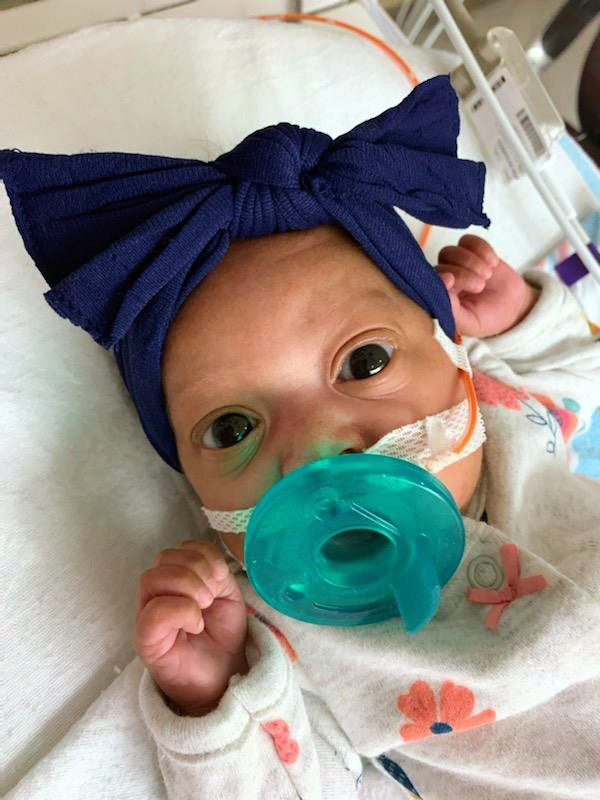
Berry underwent an emergency C-section to deliver her twins: her son, Shaquille, who weighed just 2 pounds, 6 ounces, and her daughter, Symphoni, who weighed a mere 1 pound, 15 ounces.
Like many premature infants, Symphoni was diagnosed with a patent ductus arteriosus (PDA), the persistent opening of a vessel that connects the pulmonary artery to the aorta. Typically, the PDA closes in the first few days of life, but when it does not, it often allows too much blood flow and pressure into the lungs. This is particularly problematic in premature infants who typically struggle with the immaturity of their lungs.
“Symphoni required respiratory support around the clock from different devices,” Berry said. “She was so fragile and not progressing.”
Her brother had already safely made it home, but Symphoni had not. In August, they were referred to WVU Medicine Children’s to try to repair her defect.
Alex Verhoeven, M.D., the only pediatric interventional cardiologist in West Virginia, offers minimally invasive options to close the PDA. These options include the newest device for this purpose, the Amplatzer Piccolo, built specifically for premature infants weighing as little as 1 pound, 7 ounces, an option available at select children’s hospitals in the nation.
Traditionally, surgery has been the only option for premature babies, but with the development of new devices and new skills, some interventional cardiology programs are equipped to perform less invasive techniques for premature infants who meet the appropriate criteria.
“When Symphoni arrived at WVU Medicine Children’s, she weighed about 4.4 pounds and was on a ventilator. It was clear that her delicate lungs needed help, and we discussed all the options with her family. We felt that using a catheter-based approach would allow her small body to heal faster without the whole-body impact that surgery can have on an infant so small,” Dr. Verhoeven said. “The procedure involves accessing the vein in the leg and using this tiny blood vessel as a portal to the heart. Through this small hole and with the help of both ultrasound and x-ray imaging, we are able to place a small soft, metal mesh device into the heart or blood vessel causing the problem.”
Symphoni’s PDA was closed with an Amplatzer device, allowing her to return to the Neonatal Intensive Care Unit and quickly come off all of her breathing support. Just a couple days later, she was reunited with her mother.
“I walked in, and her mother was holding her without any wires, tubes, or breathing support for the first time after being dependent on them for months,” Verhoeven said.
“Symphoni has found her voice. She is off all oxygen, she is able to bottle feed, plus her attitude and personality are starting to show. We are so grateful to Dr. Verhoeven and his team. They were more than helpful and provided excellent care,” Berry said. “I can’t wait for us all to grow together as a family.”
For more information on WVU Medicine Children’s, visit Childrens.WVUMedicine.org.
For media inquiries: Angela Jones-Knopf, Corporate Director of Media Relations and Public Affairs, 304-285-7259 - [email protected]